|
Key Takeaways:
|
Papilledema is a swelling of the optic disc caused by raised pressure around the brain, and it can threaten vision if missed. The confusing part is that early papilledema symptoms can be subtle and look like headaches, brief blur, or nausea from other causes.
In this blog, you’ll learn the causes, papilledema stages, warning signs, diagnosis, and papilledema treatment so you know when to act.
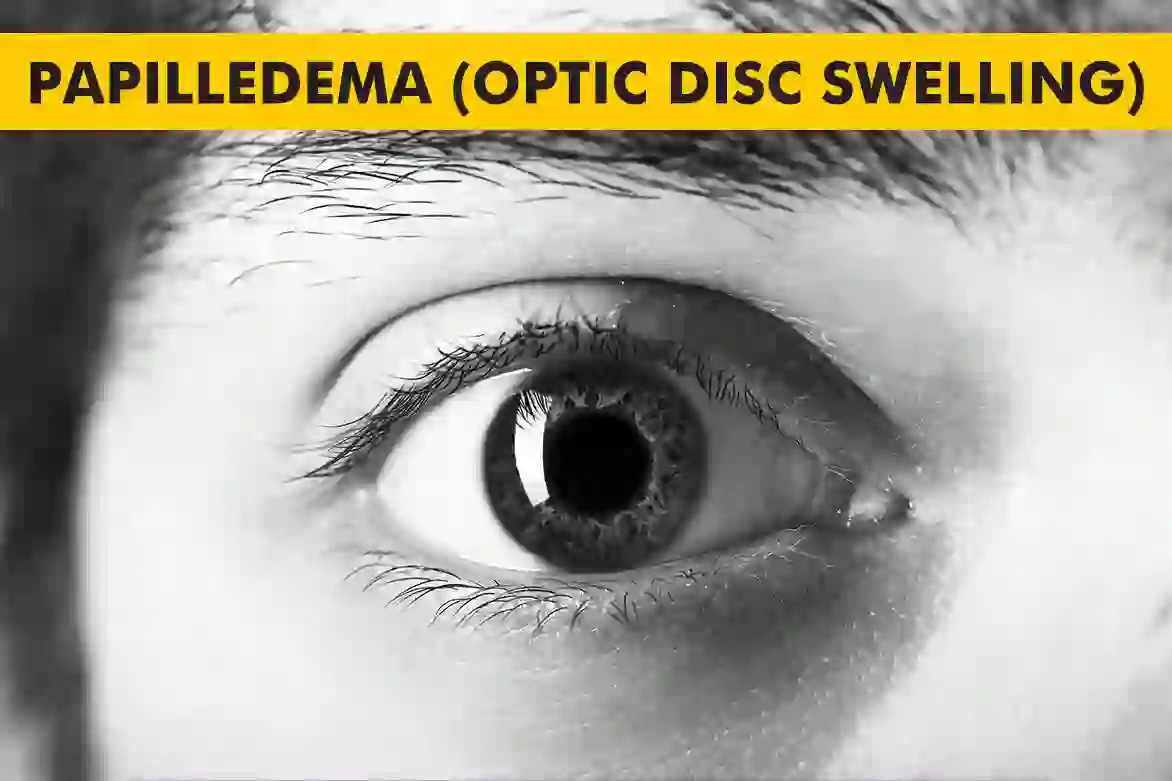
What is Papilledema?
Papilledema means swelling of the optic disc, the spot where the optic nerve meets the retina, because the pressure around the brain is too high. When that pressure rises, it travels along the optic nerve and makes the disc swell, which can blur vision, dim colors, and cause brief “grey-outs.” Papilledema is not a disease by itself; it is a warning sign that something is raising pressure inside the skull and needs prompt care. Finding the cause early protects vision and helps prevent permanent damage.
Papilledema Stages
Doctors grade papilledema (swelling of the optic disc) with the Frisen scale to track severity and guide care. The eye specialist looks at the optic disc and nearby vessels during a dilated exam with photos/OCT and assigns a stage.
- Stage 0: Disc looks normal, with a slight blur of the nasal/superior/inferior edges.
- Stage 1 (very early): Subtle swelling; the nasal border starts to look fuzzy.
- Stage 2 (early): All borders look blurred; the nasal edge is slightly elevated, and a light “halo” appears.
- Stage 3 (moderate): All borders are obscured; one or more major vessels are hidden as they cross the edge; the disc looks larger with a clear halo.
- Stage 4 (marked): The whole disc is elevated; all borders and at least one major vessel are obscured; halo persists.
- Stage 5 (severe): Dome-like bulging of the disc with loss of the normal cup, a narrow halo, and sometimes complete obscuration of major vessels.
Causes of Papilledema
Below are the causes of Papilledema:
Anything that raises cerebrospinal fluid (CSF) pressure, or blocks its flow or absorption, can swell the optic disc. Common drivers include brain tumors or masses, hydrocephalus, head injury with bleeding or brain swelling, meningitis/encephalitis, and clots in brain veins (venous sinus thrombosis). Some medicines (for example, high vitamin A/retinoids or certain antibiotics like tetracyclines) can also raise pressure.
- Brain tumours.
Both benign and malignant tumors can take up space, disturb CSF flow, and increase pressure. The effect depends on size and location; growths near CSF pathways or the brainstem are more likely to cause papilledema and headache. Treating the tumor with surgery, medicines, or other therapy helps reduce pressure and protect the optic nerve.
- Traumatic brain injury.
After falls, crashes, or sports injuries, bleeding (hematoma) or swelling (edema) elevate ICP. Even milder concussions can temporarily upset CSF dynamics, but severe injuries are more likely to cause persistent pressure problems. Warning signs, worsening headache, confusion, vomiting, unequal pupils, vision changes, need urgent evaluation.
- Meningitis and encephalitis.
Inflammation from infection can swell the brain’s coverings or tissue, raise CSF pressure, and trigger swelling of the optic disc. Fever, stiff neck, strong headache, sensitivity to light, and altered alertness travel with these infections; quick treatment reduces risks to life and sight.
- Idiopathic intracranial hypertension (IIH).
Also called pseudotumor cerebri, IIH is raised pressure with no mass or infection found on scans. It is more common in young women and links to weight gain, hormonal shifts, or certain medicines. Symptoms are daily pressure-type headache, transient visual dimming, double vision from a weak eye muscle, and pulsatile tinnitus (a “whooshing” sound).
Treating the pressure, weight management, pressure-lowering medicines, and careful eye monitoring helps prevent vision loss.
Symptoms of Papilledema
Below are the symptoms of papilledema:
- Visual disturbances.
People notice brief episodes of dim or blurred vision (transient visual obscurations), especially when standing up, bending, or coughing. Colors can look washed out, and peripheral vision slowly narrow if pressure stays high. Untreated papilledema symptoms can progress to blind spots and, in advanced cases, permanent vision loss.
- Headaches.
Headaches are common and are worse on waking, with coughing, or when lying down, patterns that suggest raised ICP. Nausea, vomiting, and a heavy “pressure” feeling can accompany the pain.
- Nausea and vomiting.
Significant pressure can irritate areas of the brain that control nausea, leading to vomiting that does not fully relieve the headache. This combination with visual changes should prompt urgent medical review.
- Pulsatile tinnitus.
A rhythmic, whooshing sound in one or both ears can occur when high pressure affects blood flow near the brain and ear structures. It gets louder when lying down and improves as pressure is treated.
Diagnosis of Papilledema
A careful eye and neurological work-up confirms what is papilledema, rules out look-alikes, and finds the cause of raised intracranial pressure. Below are the ways to diagnose papilledema:
Dilated fundus exam to see swelling of the optic disc; fundus photos and OCT measure nerve swelling; visual-field testing checks for blind spots.
- Imaging tests:
MRI of brain and orbits with MRV looks for tumors, bleeding, hydrocephalus, or venous sinus thrombosis.
- Lumbar puncture:
Measures cerebrospinal fluid (CSF) pressure and checks for infection/inflammation; done after imaging when IIH (pseudotumor cerebri) is suspected.
Treatment for Papilledema
The core of papilledema treatment is fixing the cause of papilledema and lowering pressure to protect sight.
Managing underlying causes:
Brain tumors/masses need surgery, radiation, or chemotherapy. Infections (e.g., meningitis) require targeted antibiotics or antivirals. Blood clots in the brain veins are treated per stroke protocols.
Medications:
First-line for IIH is pressure-lowering medicine such as acetazolamide; topiramate helps in selected patients. Short steroid courses are only used when there’s a steroid-responsive inflammatory cause; steroids are not routine for IIH and can worsen weight gain. Pain, nausea, and blood-pressure control are treated as needed.
Surgical Options
Below are the surgical options for Papilledema:
- Shunt Placement
A shunt is a thin tube that drains extra cerebrospinal fluid (CSF) from the brain to another part of the body (usually the abdomen) to lower pressure. Doctors consider a ventriculoperitoneal (VP) shunt when vision is at risk or medicines like acetazolamide have not worked well. The goal is to protect the optic nerve by reducing the pressure that causes papilledema.
After surgery, you’ll have regular follow-ups to check vision, headaches, and shunt function; adjustments or revisions can be needed over time.
Possible risks include infection, blockage, over-drainage (causing low-pressure headaches), or the need for future surgery, but for many patients, a well-functioning shunt stabilizes symptoms and preserves sight.
- Optic Nerve Sheath Fenestration
Optic nerve sheath fenestration (ONSF) is an eye-side procedure that creates small openings in the sheath around the optic nerve to let CSF escape locally and relieve pressure on the nerve head. It is chosen when vision is dropping quickly from papilledema, especially in idiopathic intracranial hypertension, or when one eye is worse than the other.
ONSF aims to protect vision rapidly; headaches may or may not improve because overall brain pressure can remain the same. After the procedure, vision and optic disc swelling are monitored closely, and additional treatment will still be needed.
Risks include double vision, bleeding, infection, or no visual improvement, but in experienced hands, ONSF can be a vision-saving option.
Prevention for Papilledema
Prevention focuses on lowering risk for raised pressure and catching problems early.
- Weight and health management:
For IIH, even a 5–10% weight loss can reduce pressure and symptoms; treat sleep apnea and keep blood pressure under control.
- Medication review:
Avoid or closely monitor drugs linked to raised ICP (e.g., excess vitamin A/retinoids, some tetracyclines) unless clearly needed; never start/stop medicines without medical advice.
- Follow-up and red flags:
Keep appointments if you have headaches with visual symptoms or known risk factors; seek same-day care for sudden vision dimming, transient blackouts, double vision, or pulsatile tinnitus.
Conclusion
Papilledema means the optic disc is swollen because the pressure around the brain is too high. The safest plan is simple: find the cause fast, lower the pressure, and protect vision with close follow-up. With timely diagnosis, the right medicines, and surgery when needed, most people stabilize well and keep their sight.
FAQs
What is the main cause of papilledema?
The main cause of papilledema is increased intracranial pressure (ICP) that travels along the optic nerve and makes the optic disc swell.
What is the treatment for papilledema?
The treatment for papilledema involves addressing the underlying cause of raised pressure (e.g., tumor, clot, infection, IIH) and lowering ICP with medications such as acetazolamide. If vision is at risk, procedures like shunt placement or optic nerve sheath fenestration may be employed.
What are the 4 stages of papilledema?
The 4 stages of papilledema are grouped clinically as early (roughly Frisen 1–2), moderate (Frisen 3), marked (Frisen 4), and severe (Frisen 5), moving from a subtle blur of disc edges to dome-shaped swelling with vessel obscuration.
Is papilledema a brain tumor?
No, papilledema is not a brain tumor; it is a warning sign of raised pressure that a tumor can cause, but also by clots, infections, hydrocephalus, or idiopathic intracranial hypertension.
Can papilledema cure itself?
No, papilledema can improve when the underlying pressure is brought down, but it does not safely “cure itself” without finding and treating the cause.
Which vitamin deficiency causes papilledema?
A vitamin deficiency does not cause papilledema; it is linked to raised pressure, and in some cases to excess vitamin A rather than lack of a vitamin.
Is papilledema life-threatening?
Yes, papilledema can signal a life-threatening cause of raised pressure, so it needs urgent evaluation even if symptoms seem mild.
What are the main papilledema causes?
The primary cause of papilledema is increased intracranial pressure, due to brain tumours, head trauma, infections, or idiopathic intracranial hypertension.
How is papilledema diagnosed?
Papilledema is diagnosed with a dilated eye exam and tests like OCT and visual fields, then brain imaging (MRI/MRV or CT) and sometimes a lumbar puncture to measure CSF pressure.
What are the common papilledema symptoms?
The common papilledema symptoms are headache (worse on waking or lying down), brief vision dimming, blurred vision, double vision, and pulsatile tinnitus (a whooshing sound).
Can papilledema be treated?
Yes, papilledema can be treated by lowering intracranial pressure and addressing the cause, using medicines first and surgery when vision is threatened.